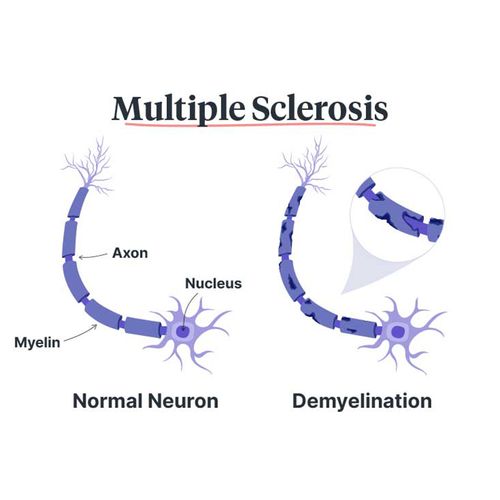
The suspension of natalizumab (Tysabri), a drug that was recently approved to treat multiple sclerosis (MS), has hampered—but not destroyed doctors' ability to combat the disease, according to experts.
"Tysabri was a promising new avenue of therapy,' says Dr. Marshall Keilson, director of neurology at Maimonides Medical Center in New York City, one center that is participating in clinical trials of the drug, "It had a different presumed mechanism of action, so we felt that we could use this in combination with other drugs and help prevent the disease in more ways than one," he adds.
What Happened
Tysabri received accelerated approval from the US Food and Drug Administration (FDA) in November 2004 after research showed it reduced relapses of MS by 66% after one year of treatment.
When combined with Avonex, another MS drug. Tysabri reduced exacerbations by 54% compared with Avonex alone.
But future trials and sales were suspended by the drug's manufacturer after one patient died of a central nervous system disorder and another patient fell ill with progressive multifocal leukoencephalopathy (PML), a rare and often fatal neurological disease that has no known treatment.
The FDA issued a public health advisory informing patients and their doctors of the suspension. Both the company and the FDA say the drug may be brought back as a treatment for MS.
Dr. Steven Galson, the acting director of the FDA's Center for Drug Evaluation and Research, says that his agency "continues to believe Tysabri offers great hope to MS patients.
Approximately 5,000 people have taken Tysabri since it was approved, reports the drug's manufacturer. An additional 3,000 people were involved in trials.
Discouraging News
"People had been very hopeful about Tysabri, called Antegren in early clinical trials, says Nicholas LaRocca, director of health-care delivery and policy research at the National Multiple Sclerosis Society in New York City. "It's discouraging that a drug that looked so promising is now in limbo."
Despite the suspension of Tysabri, "treatment for MS has not come to a screeching halt," adds LaRocca. There are other drugs on the market that, while not cures, can help slow or stabilize the disease.
The suspension "really puts into perspective short-term trials," says Keilson.
"When it was approved, everyone said, Gee, isn't it amazing that it was approved so quickly! The data was so impressive (the FDA) felt the need to approve it quickly. Now we know why the FDA needs to be more circumspect."
The Biologic Edge
Tysabri is one of a new generation of drugs called biologic therapies, engineered to target very specific mechanisms in the body. By targeting so specifically, scientists hoped to stave off unwanted side effects.
Tysabri seemed to work against MS by preventing certain immune factors from passing across the blood-brain barrier, LaRocca explains.
However, Tysabri's troubles do not necessarily condemn the larger group of biologic treatments, experts say.
"We've seen in the last few years, a tremendous surge in the utilization of biologics, and I don't think that's going to go away." Keilson says. "We just need to understand what happened with Tysabri.
Drug Keeps MS at Bay.
A European study offers more evidence that K weekly injections of interferon beta can slow the progression of multiple sclerosis (MS) in people who have early symptoms.
In the study, weekly injections of the drug reduced the loss of brain tissue in early-stage MS patients, researchers say.
Two years after treatment, only 31% of 131 patients who received interferon beta had progressed to full-blown disease, compared with 47% of 132 patients who received a placebo.
Magnetic resonance imaging (MRI) scans also showed that patients who were given the drug had significantly less brain tissue loss than those getting a placebo.
These drugs, sold as Avonex, Rebif and Betaseron, are already used to prevent relapse in people with later-stage MS.