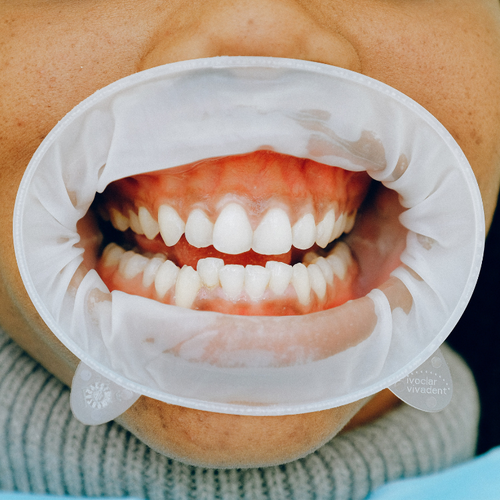
The proportion of people taking widely prescribed oral osteoporosis drugs who develop a nasty jaw condition may be much higher than previously thought, a new study suggests.
Previous reports had indicated that the risk of developing osteonecrosis of the jaw (ONJ) after taking bisphosphonates were "negligible," although there was a noted risk in people taking the higher-dose intravenous form of the drug.
ONJ is characterized by pain, soft-tissue swelling, infection, loose teeth and exposed bone.
But Parish Sedghizadeh, DDS, MS, an assistant professor of clinical dentistry at the University of Southern California School of Dentistry in Los Angeles, said his clinic is seeing one to four new cases a week, compared to one a year in the past. This led him to investigate the phenomenon and publish the findings in the Journal of the American Dental Association.
"This is more frequent than everybody would like to think it is," said Dr. Sedghizadeh, lead author of the study.
Background
Bisphosphonates are medications used to reduce the risk for bone fracture and to increase bone mass in people with osteoporosis. They're also used to slow bone "turnover" in people who have cancer that has spread to their bones, and in people who have the blood cancer multiple myeloma.
.
Use of bisphosphonates has been associated with other problems in the past, including an increased risk of atrial fibrillation (a type of abnormal heart rhythm), unusual fractures of the thigh bone, and inflammatory eye disease.
The Study
After searching the USC School of Dentistry's medical records database, the study authors found that nine of 208 patients taking the bisphosphonate alendronate (Fosamax) had active ONJ, a prevalence of about 4%. All were patients who had undergone some kind of dental procedure, such as having a tooth removed.
Fosamax is the most widely prescribed oral bisphosphonate and has been the 21st most prescribed drug in the United States since 2006, according to the study.
The jaw complication has been seen in patients taking Fosamax for as little as one year. It seems to occur most frequently after routine tooth extraction, the study authors said.
Theory
Although no one is sure why bisphosphonates seem to have this effect only on jaw bones, Dr. Sedghizadeh speculated that the drugs may make it easier for bacteria to adhere to bone that is exposed after a tooth extraction.
Previously, experts had thought that ONJ in people taking intravenous bisphosphonates was related to their underlying condition (for example, cancer), not to the actual drug, explained James Liu, MD, chairman of obstetrics and gynecology at MacDonald Women's Hospital at Case Medical Center, University Hospitals in Cleveland.
Implications
Dr. Liu said the finding "does not mean that women should stop taking the drug if they're on it. It does mean that there may be more frequent side effects than was previously known."
The USC School of Dentistry now screens every patient for bisphosphonate use.
"As a school now, we don't have complications any more, we only have referrals," Dr. Sedghizadeh said. "We put patients on anti-microbial, anti-fungal rinse one week preoperatively or postoperatively. If they have been on bisphosphonates six months or a year or longer, then we have a prevention protocol which has been very, very effective."
Manufacturer Makes Statement
According to a statement released by Merck & Co., which makes Fosamax, the new study "has material methodological flaws and scientific limitations, making it unreliable as a source for valid scientific conclusions regarding the prevalence of ONJ in patients taking alendronate."