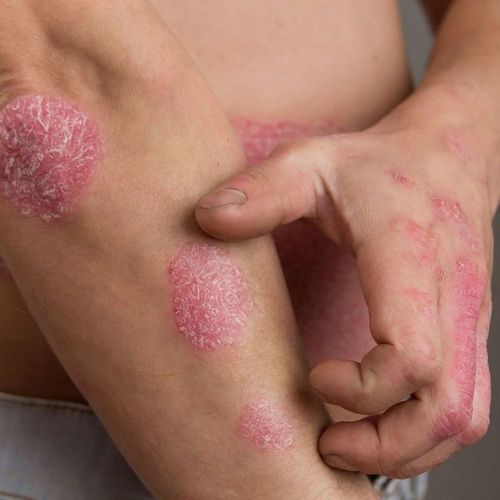
Until recently. there were few effective treatment options for 1.5 million people who have moderate to severe psoriasis, the skin condition characterized by red, scaly patches.
Now: Drugs known as biologics, made from the proteins of living cells, inhibit the immune cells that trigger psoriasis flare-ups.
Result: Reduced skin-cell buildups and inflammation in patients who have extensive psoriasis-and fewer side effects compared with older treatments.
Here's what you should know...
Causes
Psoriasis results from genetic abnormalities in the immune system. The disease occurs when killer immune cells, called T cells, target healthy skin cells rather than foreign pathogens. The attacks trigger the release of cytokines, proteins that cause the rapid proliferation of skin cells' Because sunlight has a protective effect against flare-ups, psoriasis symptoms often worsen during late fall and early winter.
Topical Treatments
Prescription topical creams and ointments are used when psoriasis affects less than 10% of the skin surface . They also can be applied to control mild flare-ups...
Steroids are the most effective topical drugs. They're applied twice daily. When used long term, strong steroids can thin the skin and cause stretch marks.
Topical retinoids, such as tazarotene (Tazorac), usually are used in combination with steroids, allowing for a lower steroid dose to be effective and reducing the risk of side effects' Retinoids can be irritating to the skin.
Warning: Topical or oral retinoids are not recommended for women who are pregnant or planning to become pregnant because they can cause serious birth defects.
Vitamin D analogues, such as calcipotriene (Dovonex), are synthetic forms of vitamin D. These creams, typically used along with a steroid, reduce skin inflammation and inhibit cell proliferation.
Phototherapy
Ultraviolet light (UV) from the sun or artificial sources can slow cell proliferation and reduce inflammation. Light therapy is a good choice for psoriasis that doesn't respond to-or is too extensive for-topical treatment.
Narrow-band ultraviolet B (UVB) phototherapy delivers light wavelengths that treat psoriasis while minimizing the rays that cause burning. Patients usually get three treatments per week. Skin clearing takes at least four to eight weeks.
Narrow-band light therapy can result in total skin clearing in some cases, but skin lesions typically return approximately four to 12 weeks after the treatments are discontinued.
Psoralen UVA- (PUVA) therapy uses ultraviolet A light and a medication (psoralen) that makes the skin more sensitive to light. PUVA is effective against severe psoriasis, but it's usually a last resort. Patients given PUVA long-term are seven to 10 times more likely to develop squamous-cell carcinoma (cancer of the upper layers of the skin).
Combination light therapy. This particular approach combines UVB light with an oral retinoid, such as acitretin (Soriatane). It's effective in 70% to 80% of cases.
Systemic Drugs
Patients who do not respond to topical treatments or phototherapy-or whose psoriasis is severe-may need oral drugs such as metbotrexate (Trexall), cyclosporine(NeoraL) or acitretin, which suppress the immune system and inhibit rapid cell division. These medications are cheaper than some of the newer psoriasis medications.
Drawback: They have a high risk of serious side effects, including organ damage. However, the damage can be managed if your physician closely monitors you.
Methotrexate can cause liver damage and a reduced white blood cell count. A patient taking methotrexate should have his/her liver biopsied every one to two years to check for liver damage. Cyclosporine can cause high blood pressure, infections and decreased kidney function. Because of the potential for kidney damage, cyclosporine is typically used for only one year. Acitretin, the only oral retinoid approved by the US Food and Drug Administration (FDA) to treat psoriasis, can thin the hair, cause dry skin and lips, cause bone abnormalities and affect liver function. Because of the risk of birth defects, women of childbearing years should not take it.
Biologics
These drugs are a new option for moderate to severe psoriasis.
TNF inhibitors. Drugs such as etanercept (Enbrel) block the action of tumor necrosis factor (TNF), an immune system chemical that triggers rapid cell division. Adalimumab (Humira) and infliximab (Remicade) are approved by the FDA to treat rheumatoid arthritis bur are often prescribed "off-label" to treat psoriasis. Approximately 50% to 80% of patients taking TNF inhibitors experience almost total clearing of their skin.
Drawbacks: TNF inhibitors are given only by injection. Side effects are tare but may include an increased risk of infection, lymphoma, neurological problems and exacerbation of heart failure.
T-cell inhibitors. Alefacept (Amevive)slows skin cell division by blocking the effects of the T cells. Approximately 20% of patients experience almost total skin clearing.
Drawbacks: Alefacept is given by intramuscular injection in the doctor's office. Side effects are rare but may include liver function abnormalities.
Efalizumab (Raptiva) is the newest biologic. It prevents T cells from triggering scaling and/or inflammation. It's injected subcutaneously (just under the skin) by patients. Approximately 30% experience almost total clearing of the skin.
Drawbacks: Side effects include flulike symptoms and low blood platelet counts. Also, psoriasis may worsen when efalizumab is stopped. Patients taking alefacept or efalizumab require regular blood rests to determine if T-cell levels have dropped, which can lead to increased risk of infection.